In 2025, the Government has established the Jawatankuasa Bersama Peringkat Menteri untuk Kos Penjagaan Kesihatan Swasta (JBMKKS) and adopt a R.E.S.E.T framework to combat the rising medical inflation in the country. One of the government initiatives through R.E.S.E.T Framework is to transform private health provider payment mechanism from fee-for-services (FFS) to Diagnosis-related Groups (DRGs) in phases.
ProtectHealth is a not-for-profit organisation under the Ministry of Health, is appointed to collect data from private hospital to support the development of a robust and representative DRG payment structure

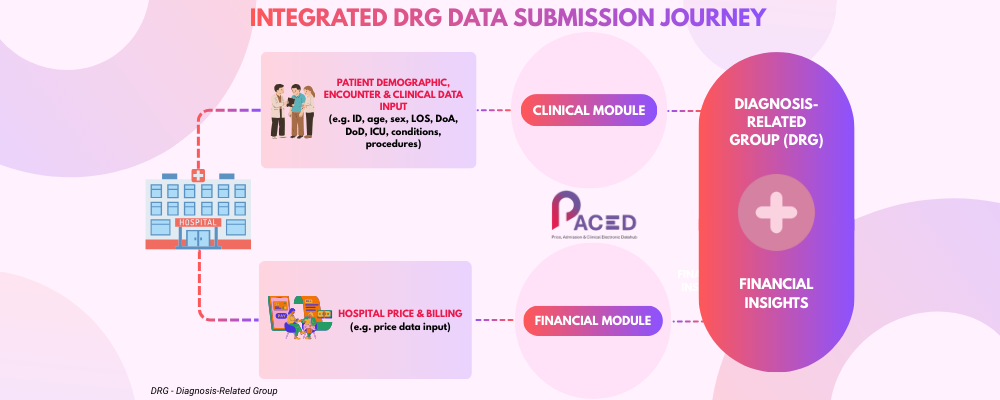
 Price, Admission & Clinical Electronic Datahub (PACED) is a system developed by ProtectHealth Corporation Sdn. Bhd. to standardize, validate, and integrate clinical and financial data across private healthcare facilities.
Price, Admission & Clinical Electronic Datahub (PACED) is a system developed by ProtectHealth Corporation Sdn. Bhd. to standardize, validate, and integrate clinical and financial data across private healthcare facilities.
PACED ensures consistent case grouping and reliable health system reporting through a structured, end to-end data journey. It enables hospitals to capture and validate clinical information, manage financial and billing data, and connect seamlessly with hospital information systems for automated data exchange.
The Project DRG training equips hospital staff with the skills to use the PACED system, covering data
standards, clinical and financial data capture, and system integration.
Module 1 – General Introduction to Project DRG (Online & Physical Sessions available)
Module 2 – Clinical Coding (Physical Sessions only)
Module 3 & 4 – PACED System Training for Clinical & Financial Users (Online Sessions only)
Module 5 – API Integration (Online Sessions only)
Module 1
Module 2
Module 3 & 4
Module 5
to be updated
The PACED System is a secure digital platform developed to support the submission of standardised clinical and billing data under Project DRG.
It enables Private Hospitals to submit admission-level data in a structured and consistent manner, supporting data quality, transparency, benchmarking, and value-based healthcare objectives.
The PACED System enables hospitals to:
Data submitted is used for analysis and private DRG payment mechanism development.
The minimum dataset for DRG collection includes:
These data must be submitted through the PACED System for all case types, payers, and participating healthcare facilities.
No patient names or personal identification numbers (e.g., IC or passport number) are required at this phase of data collection
The DRG development and data submission processes are based on internationally recognized ICD coding standards to ensure consistency, comparability, and compatibility with global DRG methodologies. For diagnoses, ICD-11 is required, with ICD-10 accepted as an interim standard during the transition period. For procedures, ICD-9-CM is the required standard. These coding systems are widely used internationally for reimbursement and health system analysis.
It is important to note that SNOMED-CT will not be used for this DRG initiative. While SNOMED-CT may continue to be used by private hospitals for internal clinical documentation and decision support, it is not compatible with DRG logic and will not be used for DRG data submissions.
We recognise that transitioning to a new clinical coding standard requires careful planning and system readiness. To ensure broad and inclusive participation, submissions using ICD-10 are accepted as an interim arrangement during this phase.
While ICD-10 remains supported in the short term, hospitals are encouraged to plan for a gradual transition to ICD-11, which will be adopted as the long-term coding standard for the DRG system. ICD-11 supports more detailed and precise clinical documentation, enabling fairer and more accurate reimbursement, particularly for complex cases. Tailored training and technical support are provided to facilitate a phased and sustainable transition.
In short, participation using ICD-10 coding is fully supported, and assistance will be available to help organisations prepare for future requirements.
Access is restricted to authorised hospital personnel.
Each hospital must appoint a Project DRG System Manager, responsible for managing access and user permissions.
Hospitals must submit a System Manager nomination form, and PACED System access will be granted once ProtectHealth approves the nomination.
The System Manager is responsible for:
The System Manager does not need to be the hospital PIC. However, the appointment must be formally approved by the hospital PIC as per CKAPS licence or by the Hospital Director / Chief Executive Officer.
The PACED System supports two user roles, both managed by the System Manager:
Clinical Users:
Financial Users:
No. Hospitals may create as many Clinical and Financial Users as needed.
Responsibility for user governance, access control, and compliance remains with the System Manager.
10. What security measures protect PACED System access?
The PACED System is safeguarded by:
These measures ensure data confidentiality, system integrity, and cybersecurity.
Hospitals must submit:
Data may be submitted via:
Detailed guidance is provided in the PACED System manuals.
To support the development of an accurate, responsive, and representative DRG model, regular data submission is strongly encouraged, preferably on a daily or weekly basis. A consistent flow of data is essential to enable timely analysis and the establishment of reliable pricing benchmarks that benefit the overall system, including participating hospitals.
All data for the preceding month should be submitted no later than the 10th of the following month. Adherence to this guideline enables efficient processing and contributes to more precise DRG modelling that accurately reflects each hospital’s clinical and financial profile.
The DRG implementation follows a carefully planned, evidence-based process to ensure accurate patient classification, fair hospital payments, and improved efficiency in care management. The first formal prospective data collection phase is planned from January onwards and will serve as the foundation for developing the initial DRG payment model. Following this initial phase, data submission is expected to transition into a continuous, ongoing process to support regular updates, recalibration, and refinement of the DRG system, ensuring it remains accurate, current, and equitable over time.
Comprehensive training and dedicated support are available to ensure smooth and accurate data submission, including guidance on clinical coding (ICD-10, ICD-11, ICD-9CM), DRG documentation best practices, and technical platform support.
It enables Private Hospitals to submit admission-level data in a structured and consistent manner, supporting data quality, transparency, benchmarking, and value-based healthcare objectives.
Yes. The platform is API-ready and designed to support seamless integration with existing Hospital Information Systems (HIS), thereby simplifying and automating the data submission process. Hospitals are encouraged to adopt this direct integration approach where feasible.
Comprehensive technical documentation, including API specifications and detailed data structures, is available to support system integration. Hospitals wishing to proceed or obtain the relevant documentation may contact the technical support team at [email protected] for further assistance.
For further information, please contact: